**
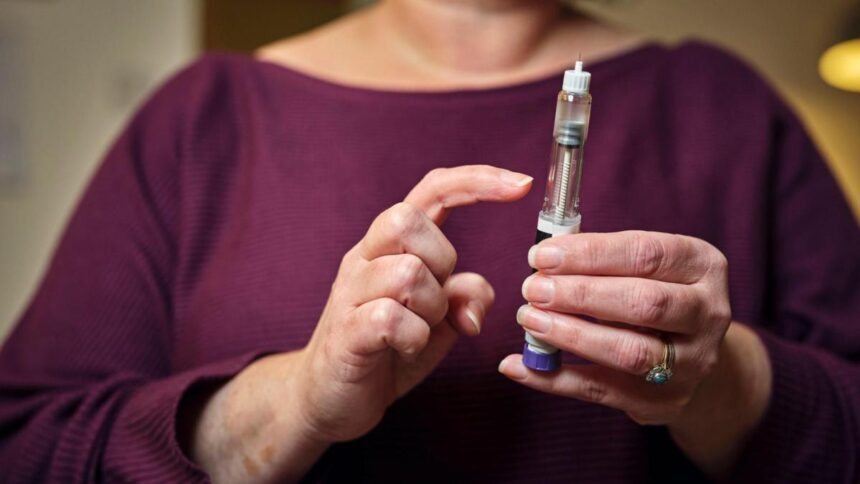
In a poignant address, Professor Sir Chris Whitty, England’s Chief Medical Officer, cautioned against the increasing dependency on weight-loss medications such as Wegovy and Mounjaro as a remedy for obesity. While recognising their transformative potential for a select few, he emphasised that relying on pharmaceuticals to manage obesity would signify a profound failure of society and the healthcare system. Sir Chris highlighted the urgent need for a cultural shift towards healthier eating habits, drawing inspiration from countries like France that have successfully maintained stable obesity rates.
The Growing Obesity Challenge
Obesity has become a pressing health concern in the UK, with approximately two-thirds of adults classified as overweight or obese. This alarming statistic has escalated over the past few decades, especially when compared to France, where obesity levels have remained relatively unchanged since the early 1990s. Sir Chris pointed out that this disparity calls for immediate action and a reevaluation of public health approaches.
During his keynote speech at the Medical Journalists’ Association annual lecture, Sir Chris articulated his concerns regarding the widespread acceptance of weight-loss drugs as a primary solution. He stated, “If a high proportion of the population ended up on the drugs, it would be a societal failure.” He cautioned against adopting a mindset that views medication as a substitute for comprehensive public health initiatives aimed at preventing obesity.
Learning from Successful Models
Sir Chris advocated for a closer examination of international practices, particularly in France, where dietary habits have fostered a healthier population. He noted that the food environments in certain areas of the UK, such as Wigan and Blackpool, are rife with junk food options, making it nearly impossible for residents to make healthier choices. “It is not the fault of people living there when presented with ‘wall to wall’ junk food,” he remarked, emphasising the need for strategic societal changes.
The professor also highlighted that reducing fat and sugar intake does not necessitate sacrificing enjoyment in food. “No one can claim the French don’t like their food,” he pointed out, encouraging the promotion of nutritious, flavourful, and affordable meals. He believes that with concerted effort, the UK can learn from successful dietary strategies employed by other countries.
The Role of Public Health Initiatives
Sir Chris underscored that the NHS currently prescribes weight-loss medications through specialised services for individuals facing significant health challenges. However, the proliferation of the private market has resulted in many people spending substantial amounts for these drugs, which raises concerns about accessibility and long-term reliance on medication.
He stressed that while weight-loss injections can be beneficial for a limited number of individuals, they should not become the default answer to obesity. “Is our answer to say ‘give up on public health’ and then just rely on drugs to get us out of a hole?” he questioned, asserting that this approach is neither socially nor medically acceptable.
Addressing the Root Causes
The aggressive marketing of unhealthy food options, particularly to children, was also a focal point of Sir Chris’s address. He noted that the health service often ends up “picking up the pieces for the rest of that child’s life” due to the detrimental effects of poor dietary choices instigated by targeted advertising.
He called for a collective societal effort to shift the focus from short-term fixes to sustainable health improvements, stating, “That is a societal choice and is one that I think we should be looking at really, very seriously.”
Why it Matters
Sir Chris Whitty’s insights highlight a crucial turning point in addressing the obesity epidemic in the UK. By advocating for a shift in focus from medication to preventive health measures, he urges society to take responsibility for fostering an environment conducive to healthy living. This approach not only has the potential to improve individual health outcomes but also to alleviate the long-term burden on the healthcare system, ultimately leading to a healthier, more resilient population.