**
Cervical cancer is emerging as Canada’s most rapidly escalating cancer, prompting urgent calls from medical experts for the federal government to intensify efforts in combating this pressing health crisis. During a press conference held on Wednesday in Ottawa, the Society of Gynecologic Oncology of Canada expressed serious concerns about the alarming rise in cervical cancer cases, despite the government’s previous commitment to eradicate it as a public health issue by 2040.
A Growing Health Concern
Dr. Shannon Salvador, the president of the Society of Gynecologic Oncology of Canada, articulated the gravity of the situation, labelling it a “silent national health crisis.” In 2025, it is estimated that around 1,650 Canadians will receive a cervical cancer diagnosis, with approximately 430 fatalities expected—a staggering figure that many experts believe is preventable.
Dr. Salvador highlighted that Canada has been heavily reliant on traditional Pap testing for cervical cancer screening, while the uptake of the human papillomavirus (HPV) vaccination has been disappointingly low. “Our initial enthusiasm for the HPV vaccine in the mid-2000s has not translated into sustained progress,” she noted, pointing to the urgent need for policy reforms to align with advancements in medical science.
HPV Vaccination Rates Stagnate
Current statistics reveal that the HPV vaccination completion rate in Canada has plateaued at a concerning 64 per cent, far short of the levels required to eliminate cervical cancer effectively. Dr. Salvador lamented that this shortfall is not merely a medical oversight but a significant policy failure.
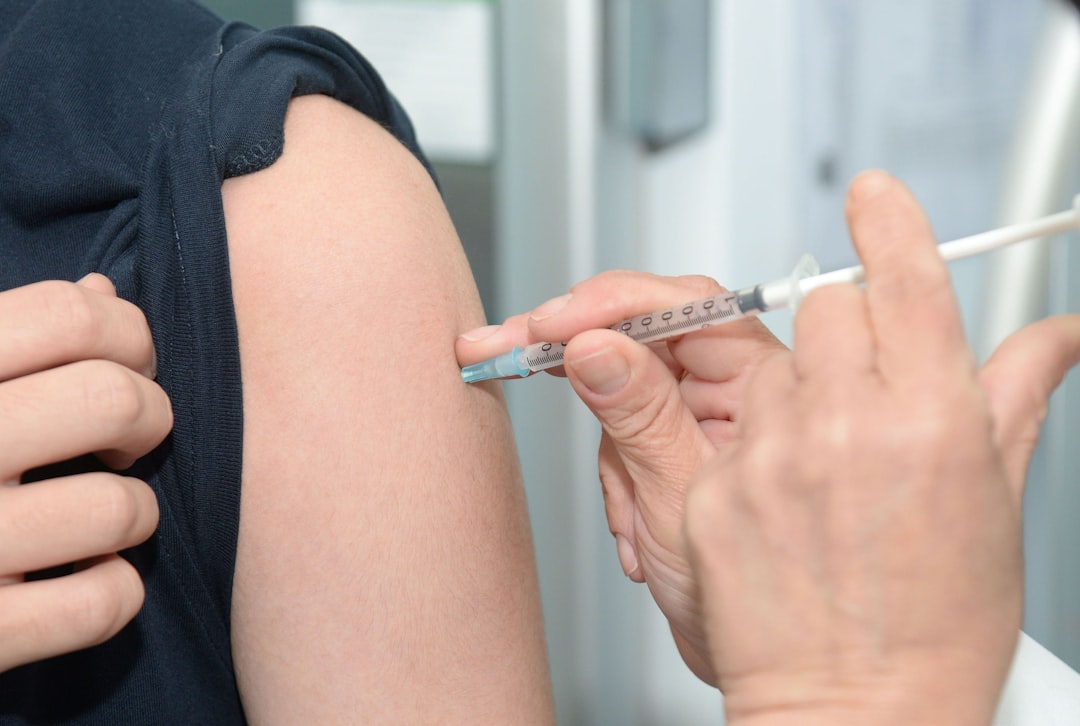
To address these challenges, the Society of Gynecologic Oncology of Canada is advocating for a nationwide pivot towards HPV DNA testing for cervical cancer screening, as well as the introduction of self-collection kits. These self-administered tests allow individuals to collect samples conveniently, thereby overcoming barriers such as geographical isolation, historical trauma, and systemic healthcare inequalities.
Addressing Systemic Barriers
Dr. Sarah Kean, the provincial lead for cervical cancer in Manitoba, emphasised that Indigenous women are disproportionately affected by cervical cancer, often facing more severe diagnoses and poorer outcomes. She attributed these disparities not to biological factors but rather to systemic issues, including lack of access to healthcare resources, geographic barriers, and entrenched racism within the healthcare system.
“Robust HPV screening must mean more than updating guidelines; it must ensure universal access across all provinces and territories, adhering to clear national standards,” Dr. Kean asserted. This comprehensive approach is vital to ensure that no one is left behind in the fight against cervical cancer.
The Cost of Inaction
The financial implications of cervical cancer are significant, with treatment costs projected to reach approximately £132 million in 2024. In contrast, implementing effective screening for eligible Canadians would total around £106 million over five years, a cost that pales in comparison to the potential human and economic toll of inaction.

As cervical cancer continues to be a leading cause of cancer death among women worldwide, the need for immediate and decisive action has never been clearer. While cervical cancer rates had previously been on a decline, recent data indicates a stagnation in progress since 2005, underscoring the urgency for renewed focus and commitment.
Why it Matters
The rise of cervical cancer in Canada represents not just a public health concern but a profound social justice issue. The barriers faced by marginalized communities, particularly Indigenous populations, highlight the systemic inequities that must be addressed to ensure equitable access to healthcare. By prioritising comprehensive HPV screening and vaccination initiatives, Canada has the opportunity to not only save lives but to rectify longstanding disparities in health outcomes. The fight against cervical cancer is not just about medical interventions; it is a call to action for a more inclusive and equitable healthcare system.