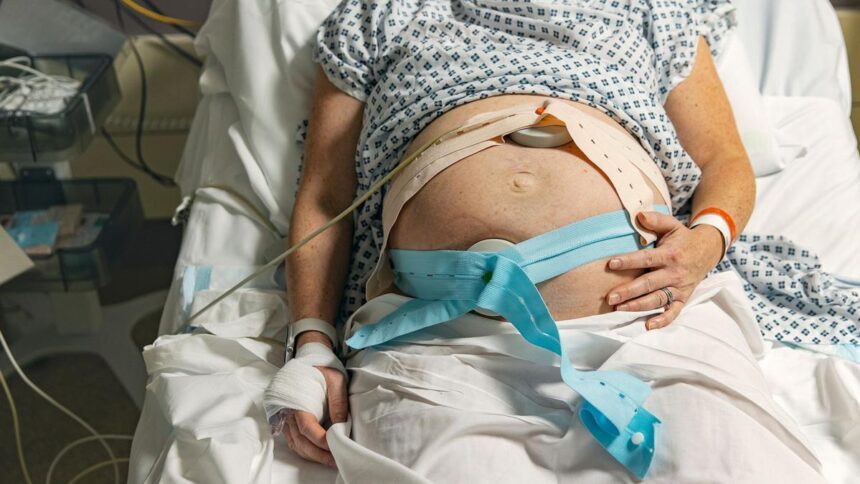
An interim report has unveiled significant shortcomings within England’s maternity services, indicating that many families are receiving inadequate care throughout the entire maternity process. The findings, led by Baroness Amos, highlight issues such as racism, staffing shortages, and a lack of accountability that have been echoed by over 8,000 individuals who shared their experiences. Health Secretary Wes Streeting has committed to implementing the final recommendations of the review, which are expected by April.
Critical Findings of the Report
Baroness Amos has conducted extensive consultations, meeting with more than 400 families to gather firsthand accounts of their experiences. Her findings suggest that the quality of care varies dramatically, with some families reporting excellent support while others endure distressing neglect.
“I have witnessed both commendable and appalling care existing side by side,” Baroness Amos stated during an interview with BBC Breakfast. “While safe and quality care is available, far too many examples of poor service persist.” The inconsistencies in care highlight the pressing need for systemic changes within the NHS.
The Roots of Discrimination in Care
One of the most alarming aspects of the report is the prevalence of racism and discrimination within maternity care. The interim findings noted that stereotypes are often perpetuated in maternity and neonatal services. For instance, Asian women are sometimes unfairly labelled as ‘princesses’, suggesting they are overly demanding, while Black women have been dismissed as having ‘tough skin’, leading to inadequately managed pain relief. Additionally, Muslim families reported feeling uncomfortable voicing concerns due to fears of bias affecting the treatment of their infants.

Baroness Amos emphasised that the report did not just highlight individual cases but pointed to systemic issues that lead to negative outcomes for women from Black and Asian backgrounds, as well as those from socio-economically deprived areas. Reports of discrimination against disabled women, refugees, and LGBT families further underscore the urgent need for reform.
Staffing Shortages and Poor Relationships
The report identified several critical areas needing attention, including staffing shortages that have left maternity units unable to provide safe care. Problems such as overcrowding in antenatal wards and delays in admissions have been exacerbated by the use of community midwives in delivery units, raising safety concerns.
Moreover, the report pointed out “poor relationships” among team members, particularly between obstetricians and midwives. Instances of racism and bullying by senior clinicians often go unaddressed, contributing to an unhealthy work environment. Baroness Amos noted, “It is evident from the conversations I’ve had that maternity and neonatal services in England are failing too many women, babies, families, and staff.”
Calls for Systemic Change
As the review progresses, many families impacted by inadequate care are demanding an independent investigation into the broader issues within maternity services. Robyn Davis, whose infant son Orlando died shortly after birth due to staff oversight, expressed her frustration: “Not listening to my concerns is the main reason we’re sat here without our son.” Her husband, Jonathan, echoed this sentiment, asserting that a cultural shift is needed in how maternity care is approached.
Their family is part of the campaign group Truth for Our Babies, advocating for comprehensive reforms to prevent future tragedies. The Davises believe that the Amos review is insufficient and are urging for a statutory inquiry that goes beyond surface-level issues.
MP Michelle Welsh has also raised concerns, suggesting that without decisive action, the review may fail to effect meaningful change. She advocates for the establishment of a maternity commissioner to ensure accountability and improvement in services. “This inquiry must yield bold policies that demonstrate the government’s commitment to enhancing maternity services,” she stated.
Despite promises from Health Secretary Wes Streeting to chair a maternity taskforce, reports indicate that this initiative has yet to materialise. Welsh emphasised the urgency of establishing this taskforce, asserting that without it, the sector lacks the driving force necessary for significant reform.
Why it Matters
The findings of this review underscore the urgent need for reform in England’s maternity services, as they reveal systemic failures that have led to tragic outcomes for families. The current state of care not only undermines the health and safety of mothers and their babies but also erodes trust in the healthcare system. As families continue to advocate for accountability and reform, the stakes are high; ensuring that future generations do not have to endure the same harrowing experiences is imperative. The government’s response to these findings will be crucial in determining the future of maternity care in England, and it is a moment that demands both attention and action.