Cervical cancer is emerging as Canada’s most rapidly increasing cancer type, prompting urgent calls from medical professionals for enhanced federal intervention. During a press conference held in Ottawa on Wednesday, the Society of Gynecologic Oncology of Canada (GOC) highlighted the critical need for improved strategies to combat what they describe as a “silent national health crisis.” This plea comes despite the Canadian government’s action plan, launched in July 2025, which aims to eradicate cervical cancer as a public health issue by 2040.
A Distressing Trend
Dr. Shannon Salvador, the president of the GOC, expressed grave concerns about the current trajectory of cervical cancer diagnoses in the country. In 2025, it was projected that approximately 1,650 Canadians would be diagnosed with the disease, with 430 succumbing to it—cases that she firmly believes could be avoided.
“Canada is currently facing a silent national health crisis,” Dr. Salvador stated, emphasising that despite notable advancements in medical science, cervical cancer remains a worrying exception. The reliance on traditional Pap testing and a stagnating rate of human papillomavirus (HPV) vaccinations are seen as significant contributors to this alarming trend.
The HPV Vaccine Gap
Currently, Canada’s HPV vaccination completion rate rests at a mere 64 per cent, a figure that Dr. Salvador points out is drastically insufficient for achieving the goal of eliminating cervical cancer. “This statistic is not just a medical failure; it is a policy failure,” she remarked, underscoring the urgent need for systemic change.
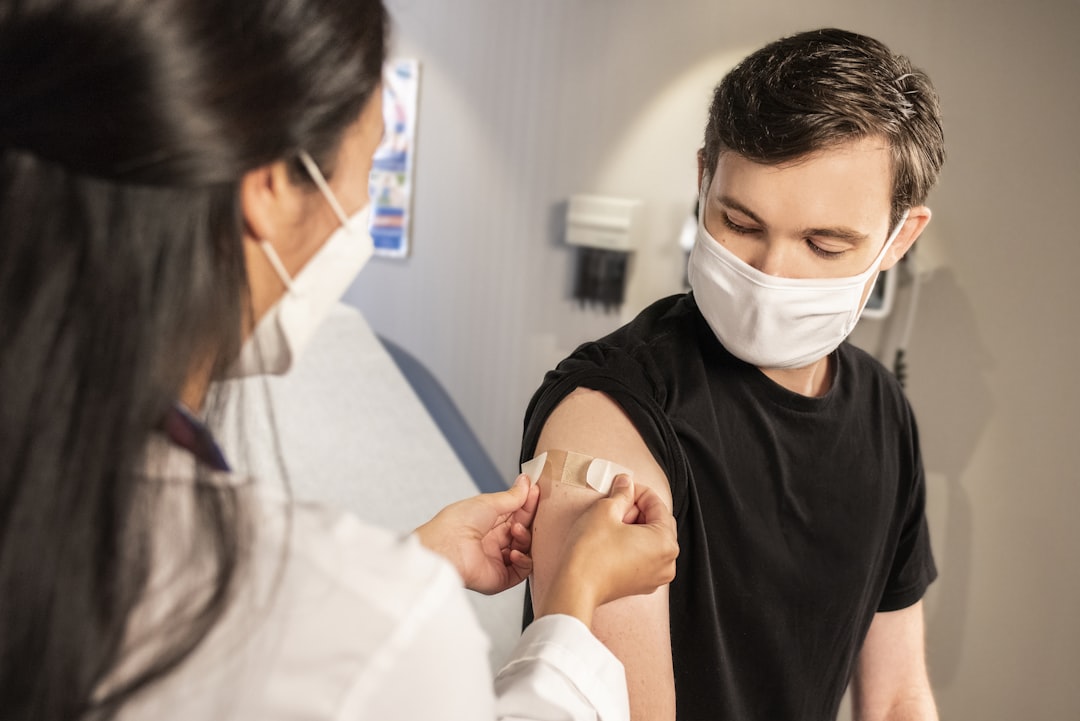
To address these challenges, the GOC is advocating for an immediate shift towards HPV DNA testing for cervical cancer screening. They are proposing the introduction of self-collection swabs and kits to facilitate easier screening access. According to the Canadian Cancer Society, HPV testing can be performed through a swab that collects cells from either the cervix or the vagina, with self-administered options available for those who may face barriers to conventional testing.
Addressing Health Inequities
The initiative to implement self-collection kits comes in light of existing disparities in healthcare access, particularly among rural, Indigenous, and underserved communities. Dr. Sarah Kean, provincial lead for cervical cancer in Manitoba, highlighted the increased rates of diagnosis and advanced disease stages faced by Indigenous women, attributing these outcomes not to biological factors but to systemic barriers.
“Indigenous women are diagnosed at higher rates, with more advanced disease, and they experience worse outcomes. This is not due to biology; it is due to barriers, lack of access to screening resources, geographic isolation, systemic racism in healthcare, and poverty stemming from colonial practices,” she explained. Dr. Kean advocates for robust, accessible HPV screening across all provinces and territories, calling for federal legislation to support these efforts.
The Economic Burden
The economic implications of cervical cancer are also significant. Dr. Salvador noted that the treatment cost for cervical cancer is projected to be $132 million in 2024, while the expense for screening eligible Canadians over the next five years is estimated at $106 million. With the World Health Organization’s global strategy aiming for cervical cancer elimination, Canada’s progress appears to have stalled, as highlighted in a report by the Canadian Cancer Society.

Despite a historical decline in cervical cancer rates from 1984 to 2005, the progress has dramatically slowed, with a negligible annual decrease of 0.3 per cent observed between 2005 and 2021. Dr. Kean pointed out that while other cancers in Canada are showing a downward trend, the one cancer that is entirely preventable continues to rise.
Why it Matters
The increasing rates of cervical cancer in Canada raise pressing concerns that extend beyond the realm of public health; they strike at the heart of healthcare equity and access. This situation represents a crucial moment for policymakers, healthcare professionals, and advocates to come together and address the systemic failures that have allowed this preventable disease to proliferate. Without immediate and comprehensive action, many Canadians, particularly those in marginalized communities, will continue to face unnecessary risks to their health and wellbeing. The time for change is now, as the health of an entire generation hangs in the balance.