Cervical cancer is emerging as a significant public health concern in Canada, with medical professionals labelling it a “silent national health crisis”. At a recent press conference held by the Society of Gynecologic Oncology of Canada in Ottawa, experts urged the federal government to intensify efforts to combat this growing issue, despite an action plan unveiled in July 2025, aiming to eradicate cervical cancer as a public health problem by 2040.
A Growing Threat
Dr. Shannon Salvador, the president of the Society of Gynecologic Oncology of Canada, expressed deep concern over the alarming statistics related to cervical cancer. In 2025, it is projected that approximately 1,650 Canadians will be diagnosed with the disease, leading to an estimated 430 deaths. Dr. Salvador highlighted the tragic irony that these fatalities are largely preventable.
“Canada is currently facing a silent national health crisis,” she stated, pointing to the inadequacies in the current screening and vaccination programmes. The reliance on Pap tests has proven insufficient, and vaccination rates against human papillomavirus (HPV), a primary cause of cervical cancer, remain worryingly low.
Stagnant Vaccination Rates
Despite initial enthusiasm for the HPV vaccine following its introduction in the mid-2000s, completion rates have stagnated at only 64 per cent nationwide. Dr. Salvador described this as not merely a failing of medical practice, but a significant policy oversight.
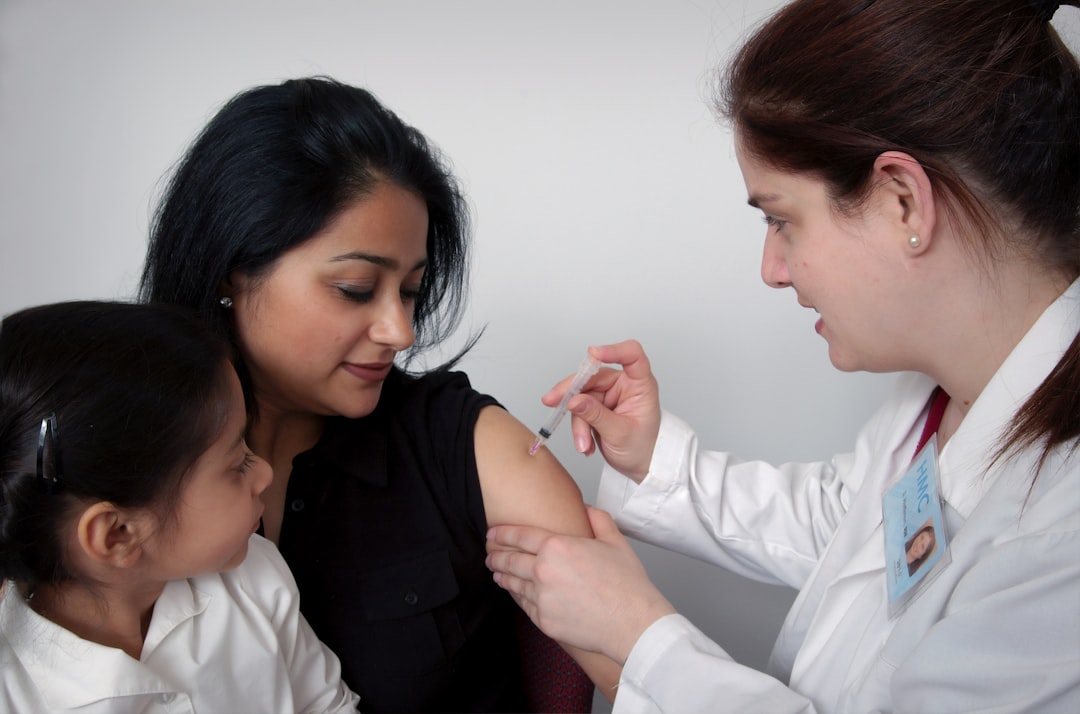
“This statistic is not just a medical failure; it is a policy failure,” she emphasised, calling for a reassessment of current strategies to enhance vaccination outreach and effectiveness.
The Society is advocating for an “immediate, national shift” to incorporate HPV DNA testing for cervical cancer screening and the implementation of self-collection kits to facilitate easier access for individuals.
Innovative Screening Solutions
Currently, HPV testing is performed through clinical swabs, either from the cervix or vagina. The Canadian Cancer Society has noted the availability of self-collected testing, where individuals can gather samples from the vagina using a swab. This method could significantly reduce barriers to screening, particularly for those facing geographical, cultural, or systemic obstacles.
Dr. Salvador pointed out that these self-collection kits can help eliminate barriers related to travel, trauma histories, and the lack of access to a family doctor, especially for individuals from rural, Indigenous, and underserved communities.
“Indigenous women, in particular, are diagnosed at higher rates and often present with more advanced disease due to systemic barriers,” warned Dr. Sarah Kean, provincial lead for cervical cancer in Manitoba. She emphasised that these disparities are not biological but stem from socio-economic factors and a fragmented healthcare system.
Calls for Comprehensive Legislative Action
The experts are calling for robust, accessible HPV screening across Canada, coupled with federal legislation to support these initiatives. Dr. Kean remarked that effective screening encompasses more than merely updating guidelines; it necessitates universal access to primary HPV testing across all provinces and territories, accompanied by clear national standards.
“Cervical cancer is one of the most preventable cancers,” she stated, urging for immediate action.
Recent reports indicate that the financial burden of treating cervical cancer on the Canadian healthcare system reached £132 million in 2024, while screening eligible Canadians would cost approximately £106 million over five years.
Why it Matters
The rising incidence of cervical cancer in Canada highlights a critical need for systemic change within the healthcare system. As the nation grapples with a preventable disease, the call for improved screening, vaccination, and legislative support becomes urgent. Addressing these gaps will not only save lives but also reduce healthcare costs and ensure equitable access to healthcare resources for all Canadians. The conversation around cervical cancer must evolve into decisive action, as every statistic represents a life impacted by a disease that should be preventable.