**
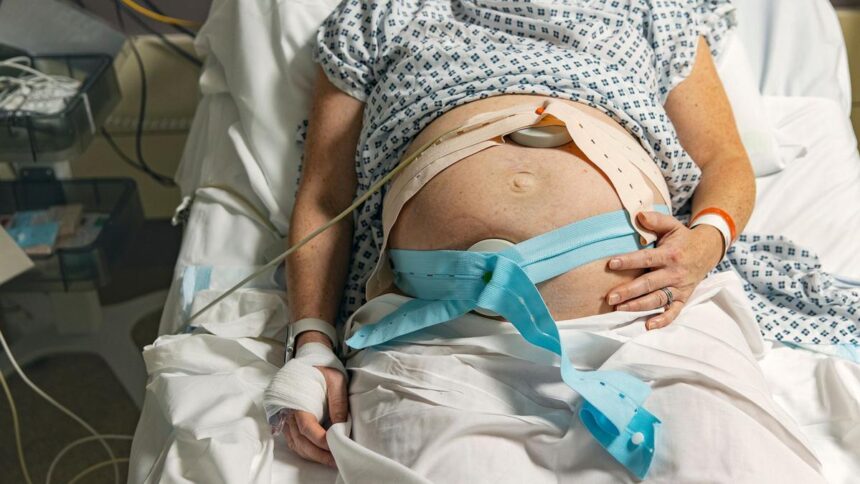
A recent interim report has revealed alarming deficiencies within maternity services across England, highlighting the distressing experiences faced by families during childbirth. Conducted by Baroness Amos as part of a government-commissioned review, the report identifies racism, inadequate staffing, and lack of accountability as key contributors to these systemic failings. With over 8,000 testimonies collected, the findings underscore the urgent need for reform in the NHS’s maternity care.
Systemic Issues Unveiled
The report outlines that maternity services are failing “too many” families, with issues evident at every phase of the maternity journey. Baroness Amos noted that her investigation has unearthed a stark contrast in care quality, stating, “I have seen bad, poor, good and excellent care co-existing side by side.” Her discussions with more than 400 families have revealed a troubling inconsistency in experiences, with many feeling traumatized by their encounters with the healthcare system.
Baroness Amos has categorically stated that while there are examples of safe and compassionate care, the prevalence of poor care is unacceptable. “What I have heard from families is so traumatic and distressing,” she remarked. The report highlights urgent areas for improvement, including the need for better relationships among healthcare professionals and a commitment to addressing the impacts of racism and discrimination within the system.
Racism and Discrimination in Maternity Care
One of the most striking findings of the report is the prevalence of racism within maternity services. It details how stereotypes are often applied to women from Black, Asian, and minority ethnic backgrounds, with accounts of Asian women being labelled as ‘princesses’ and Black women described as having ‘tough skin.’ Such prejudices can lead to inadequate pain management and a lack of understanding regarding individual needs.

Muslim families, too, have reported feeling discriminated against, often fearing that voicing concerns may result in adverse treatment for their newborns. This systemic discrimination not only jeopardises the quality of care provided but also places additional emotional burdens on families already navigating the challenges of childbirth.
Key Areas of Concern
Baroness Amos identified six critical areas contributing to the failings in maternity care:
1. **Staffing Shortages**: Many maternity units are grappling with insufficient personnel, leading to compromised safety and care quality.
2. **Poor Team Dynamics**: Relationships among healthcare professionals, including midwives and obstetricians, are often strained, with incidents of bullying and unaddressed racist behaviour.
3. **Structural Inequalities**: Women from Black and Asian backgrounds, as well as those from deprived areas, face significantly higher risks of adverse outcomes.
4. **Lack of Compassion**: Families experiencing baby loss often report insufficient support and transparency, compounding their trauma.
5. **Inadequate Facilities**: Many maternity wards operate from outdated and poorly maintained buildings, which can hinder effective clinical care.
6. **Failure to Learn from Mistakes**: A culture of blame prevails, where mothers may internalise guilt for adverse outcomes, preventing critical learning opportunities for healthcare providers.
Baroness Amos emphasises the need for immediate action, stating, “It is clear from the meetings and conversations I have had with hundreds of women, families, and staff members across the country, that maternity and neonatal services in England are failing too many.”
Families Demand Accountability
The experiences of families affected by these systemic issues are deeply poignant. The case of Orlando Davis, who died shortly after birth due to a lack of timely intervention, exemplifies the dire consequences of inadequate care. His mother, Robyn, expressed her belief that dismissing her concerns during labour contributed to the tragedy, highlighting a broader cultural issue within maternity services where practitioners may not listen to the voices of the mothers they serve.

Robyn and her husband, Jonathan, advocate for a statutory inquiry into maternity services at their local NHS Trust, arguing that the current review led by Baroness Amos lacks the depth required to instigate meaningful change. “It’s not just what’s happening at these hospitals; it’s the regulators as well,” Jonathan stated, urging for a comprehensive investigation into the systemic failures that have persisted for too long.
Calls for Urgent Reform
Labour MP Michelle Welsh has echoed these sentiments, warning that the Amos review could fall short of its potential impact if not followed by decisive government action. Welsh advocates for the establishment of a maternity commissioner to oversee improvements and ensure accountability within the system. “This inquiry must result in some big, bold policies regarding maternity services,” she insisted.
Health Secretary Wes Streeting has pledged to implement the review’s final recommendations, expected in April. However, the establishment of a maternity taskforce to drive this change has yet to materialise, raising concerns about the commitment to reform.
Why it Matters
The findings of this report serve as a wake-up call for England’s healthcare system, revealing a troubling landscape where systemic racism and inadequate staffing compromise the safety and well-being of mothers and their babies. The voices of families affected by these issues must be prioritised to ensure that future generations do not face the same harrowing experiences. Immediate and robust actions are essential to restore trust in maternity services, providing families with the compassionate, high-quality care they rightfully deserve.