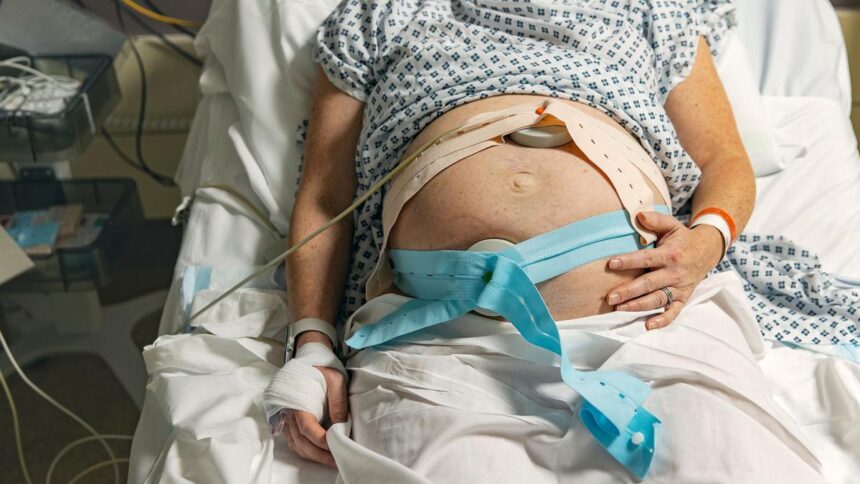
An interim report into the state of maternity care in England has unveiled alarming deficiencies, indicating that many families are receiving inadequate support throughout their maternity journey. Led by Baroness Amos, this government-commissioned review highlights issues such as racism, poor staffing, and lack of accountability as key contributors to these failures. With over 8,000 pieces of evidence submitted and discussions with more than 400 families, the report paints a troubling picture of the current state of maternity services.
Key Findings of the Interim Report
Baroness Amos’s investigation has identified six pressing areas of concern that require immediate attention.
1. **Capacity Strains on Services**: Many maternity units are struggling with insufficient resources, leading to delays in admissions and compromised safety, particularly in antenatal wards and delivery units. The reliance on community midwives in these settings has added to the strain.
2. **Interpersonal Issues Among Staff**: There exists a troubling dynamic between healthcare team members, including midwives and obstetricians. Reports of racism and bullying from senior clinicians have often gone unaddressed, exacerbating the already fragile relationships within teams.
3. **Systemic Inequalities**: The report highlights the stark disparities faced by women from Black and Asian backgrounds, as well as those from economically disadvantaged areas. Structural racism and discrimination against disabled women, Muslim families, refugees, and LGBTQ+ families have led to significantly higher risks of adverse outcomes.
4. **Lack of Compassion and Transparency**: Families experiencing baby loss often feel unsupported, with inadequate communication compounding their trauma. This lack of transparency can prevent learning from past mistakes, perpetuating a cycle of poor care.
5. **Inadequate Facilities**: Many maternity units operate in outdated and poorly maintained buildings, which can compromise care quality. The absence of suitable bereavement spaces further illustrates the neglect within some trusts.
6. **Staffing Shortages**: Many maternity units are reporting critical understaffing, impeding their ability to provide safe and effective care.
Baroness Amos has voiced her deep concern, stating, “It is clear from the meetings and conversations I have had with hundreds of women, families, and staff members across the country, that maternity and neonatal services in England are failing too many women, babies, families, and staff.”
Family Experiences Highlight Systemic Issues
The report’s findings resonate deeply with families who have suffered due to the inadequacies in maternity care. Personal accounts, such as that of the Davis family, underscore the urgent need for reform. Their son, Orlando, tragically died shortly after birth due to a failure in care related to his mother’s condition, hyponatremia. Robyn Davis, Orlando’s mother, expressed her heartache, stating, “Not listening to my concerns is the main reason we’re sat here without our son.”
The couple is part of a larger movement, Truth for Our Babies, advocating for an independent investigation into the University Hospitals Sussex NHS Trust. They argue that the current review lacks the depth required to enact meaningful change across the board.
Calls for Accountability and Action
Political figures, such as Labour MP Michelle Welsh, are echoing the sentiment for decisive government action. Welsh warns that without substantial reforms, the Amos review risks being ineffective. She advocates for the establishment of a maternity commissioner to ensure accountability and facilitate improvements in care standards.
Health Secretary Wes Streeting has committed to acting on Baroness Amos’s final recommendations, expected in April, and has pledged to lead a maternity taskforce aimed at driving enhancements in service delivery. However, concerns have been raised about the taskforce’s delay in formation, with Welsh urging for its swift establishment to generate impactful policy changes.
Why it Matters
The revelations within this interim report expose the vulnerabilities in England’s maternity services, highlighting a pressing need for systemic reform. With countless families affected and lives at stake, the urgency for accountability and compassionate care has never been clearer. As the health sector grapples with these challenges, the hope remains that forthcoming recommendations will pave the way for a safer, more equitable maternity experience for all families in the future.