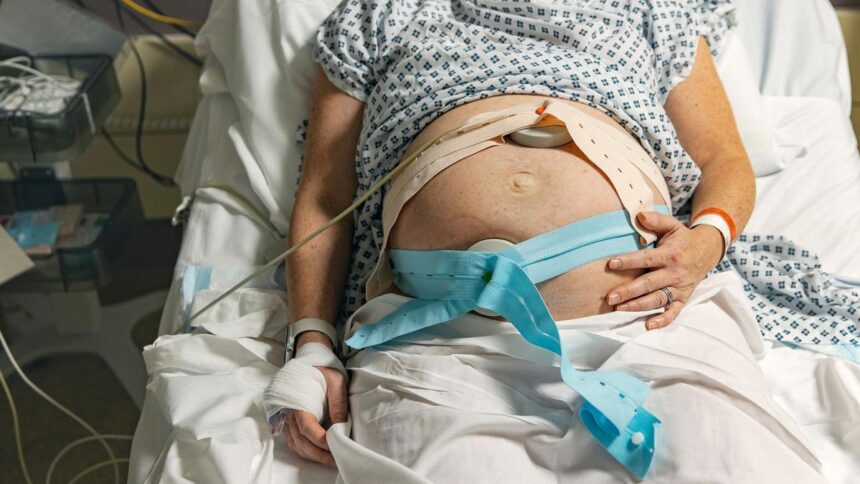
An interim report led by Baroness Amos has revealed significant failings within England’s maternity services, affecting far too many families during their critical journey into parenthood. The review, commissioned by the government, has identified a range of issues including systemic racism, inadequate staffing, and failures in accountability that have plagued maternity care across the country. With over 8,000 testimonies gathered and meetings held with more than 400 families, this investigation aims to address the inconsistencies and disparities in care delivery.
Critical Findings of the Review
Baroness Amos’s interim report sheds light on six major areas of concern within the maternity services framework. These findings underscore the urgent need for reform:
1. **Capacity Issues**: Many maternity wards are operating beyond their limits, leading to delays in patient admissions. The reliance on community midwives in delivery units has raised safety concerns.
2. **Team Dynamics**: The report highlights “poor relationships” among healthcare professionals, particularly between obstetricians and midwives. Instances of racism and bullying behaviour from senior clinicians were noted, often going unaddressed by management.
3. **Racial and Socioeconomic Disparities**: Women from black and Asian backgrounds and those from deprived areas experience a notably higher risk of adverse outcomes. The review also documented discrimination against disabled women, Muslim families, refugees, and LGBTQ+ individuals.
4. **Compassionate Care Deficiencies**: When faced with baby loss or harm, families reported a lack of compassion and transparency from healthcare providers. This not only compounds trauma but also hampers learning opportunities from past mistakes.
5. **Inadequate Facilities**: Many maternity services are housed in outdated and poorly maintained buildings, which can compromise the quality of clinical care. In some cases, bereavement spaces were either insufficient or entirely absent.
6. **Staffing Shortages**: A significant number of staff reported that maternity units lacked adequate personnel to ensure safe care, raising alarms about the sustainability of current practices.
Baroness Amos emphasised the mixed nature of care being provided across the NHS. “I have seen bad, poor, good and excellent care co-existing side by side,” she stated. Her observations reflect the traumatic experiences shared by families, revealing a patchwork of care that varies drastically from one trust to another.
Family Voices Demand Accountability
The findings resonate deeply with families who have faced devastating outcomes due to these systemic failings. One poignant case is that of Orlando Davis, who tragically died just 14 days after birth due to failures by staff at Worthing Hospital in Sussex, who overlooked his mother’s dangerously low sodium levels during labour. His mother, Robyn, expressed her anguish, stating, “Not listening to my concerns is the main reason we’re sat here without our son.”
The Davis family is part of a group advocating for an independent inquiry into maternity services at the University Hospitals Sussex NHS Trust. They fear that the current review led by Baroness Amos may not be comprehensive enough to address the systemic issues thoroughly. “It’s not just what’s happening at these hospitals; it’s the regulators as well,” Jonathan Davis remarked, highlighting the need for a broader investigation that encompasses all facets of maternity care.
Calls for Bold Policy Changes
Labour MP Michelle Welsh, who has been vocal about maternity safety, warned that the Amos review risks being ineffective unless it leads to substantial policy changes. She advocates for the establishment of a maternity commissioner to oversee improvements in care. “This inquiry must result in some big, bold policies that really say that as a government we want to improve maternity services,” she urged.
Despite Health Secretary Wes Streeting’s promise to chair a taskforce aimed at driving enhancements in maternity care, it has come to light that this group has yet to be established. Welsh expressed concern, stating, “It is important that the taskforce is established as soon as possible, because without it we don’t have that driving force.”
Why it Matters
The implications of this report extend beyond statistics and policy recommendations; they resonate deeply with families navigating one of life’s most profound experiences. The failings in maternity care not only leave lasting impacts on mothers and their babies but also erode trust in the healthcare system. As Baroness Amos continues her work, the hope is that her final recommendations will spark meaningful change, ensuring that future generations receive the safe, compassionate care they deserve. The call for accountability and systemic reform is not just a request for better services—it is a demand for a fundamental respect for the lives and experiences of families across England.