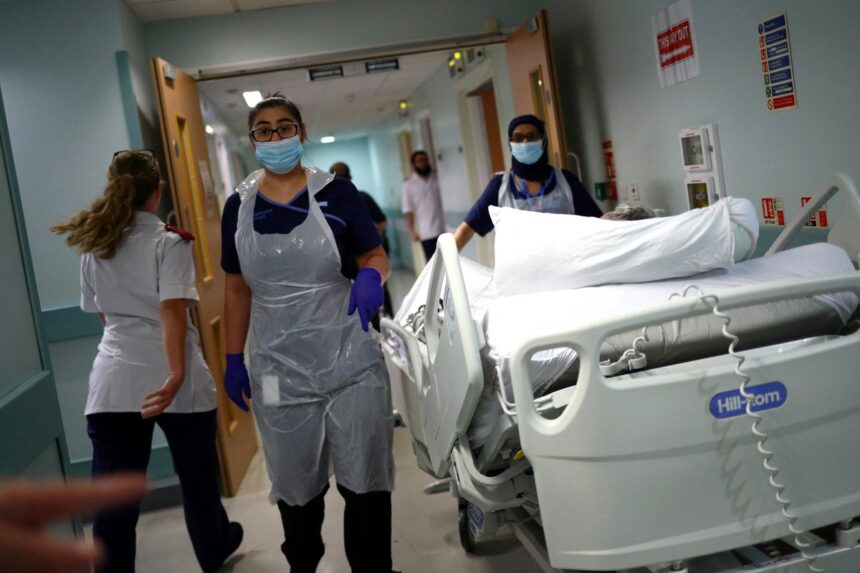
The National Health Service (NHS) is currently in a precarious condition, with top medical professionals cautioning that it would struggle to manage a new pandemic. Despite having endured the catastrophic impact of COVID-19, health leaders have expressed serious concerns over overcrowded hospitals and an alarming rise in waiting lists, indicating that the health service is in a significantly worse position than it was prior to the pandemic. As the UK Covid Inquiry prepares to unveil its findings, the stark realities of the healthcare system’s vulnerabilities are coming to light.
Current State of the NHS: A Troubling Landscape
The NHS is grappling with a multitude of pressures that have compounded since the pandemic. Emergency departments are inundated, and the phenomenon of corridor care—where patients are treated in hallways due to a lack of space—has surged alarmingly. According to NHS data, more than 71,500 patients waited over 12 hours in Accident & Emergency departments in January 2026—a staggering increase from just 627 in January 2019. Furthermore, the waiting list for surgeries has climbed to an unprecedented 7.2 million, up from 4.27 million just a few years earlier.
Dr Ian Higginson, president of the Royal College of Emergency Medicine, articulated the dire situation, stating, “From our perspective, our departments are much more overcrowded, and our hospitals are under even more pressure than they were before.” He emphasised that the system’s fragility means it is ill-prepared for another sudden surge in patient numbers akin to what was witnessed during the peak of COVID-19.
Lessons Unlearned: A Call for Preparation
As the Covid Inquiry, led by Baroness Heather Hallett, prepares to release its report, there is a palpable sense of urgency among health leaders who assert that the lessons from the last pandemic have not been adequately integrated into future planning. Dr Shondipan Laha, president of the Intensive Care Society, expressed concern that the knowledge acquired during the pandemic is fading rapidly, stating, “It’s not just about being ready for a pandemic. It’s being ready for a war.”

Former NHS England medical director Sir Stephen Powis previously voiced fears that the health system could become overburdened again, noting the rationing of care during the last crisis. There is a growing consensus that the national mechanisms established to track critical care bed availability have fallen by the wayside, leaving the NHS vulnerable to future crises.
Dr Laha highlighted a troubling trend where some trusts are considering reducing ICU bed numbers due to financial constraints. This decision-making process, she argues, could have devastating consequences for patient care during times of emergency.
The Human Cost: Burnout and Staff Shortages
Compounding these systemic issues is the pervasive burnout among NHS staff, who are reportedly facing unprecedented levels of fatigue. Dr Vicki Price, president of the Society of Acute Medicine, noted that while healthcare workers rose to the challenge during the pandemic, the toll it has taken on their mental and physical well-being is substantial. A recent NHS staff survey revealed that over a third of employees feel burnt out, with only 32 per cent believing they have sufficient staffing levels to provide adequate care.
Dr Laha warned that the repercussions of another pandemic would likely fall heavily on already overstretched healthcare professionals. “We would have to cope, but it would come at the expense of our staff,” she said, emphasising the human cost of neglecting proper support and resources.
Preparing for the Future: A Systematic Approach Needed
The findings from the forthcoming inquiry will be critical in evaluating the NHS’s response and readiness for any future health emergencies. Health leaders are calling for a comprehensive, system-wide strategy that addresses not only pandemic preparedness but also the ongoing challenges within the social care sector, which they describe as “completely broken.”

Professor Mumtaz Patel, president of the Royal College of Physicians, lamented the current lack of coordinated pandemic planning, stating, “I do feel that preparedness is not there.” The need for proactive measures to ensure the NHS can withstand future pressures is more pressing than ever.
Why it Matters
The current state of the NHS is not merely a reflection of past failures; it serves as a critical indicator of how societies must prepare for future public health crises. As the world continues to face the repercussions of COVID-19, the lessons learned—or ignored—will shape the resilience of healthcare systems globally. Ensuring that the NHS is adequately equipped to handle future emergencies is not just a matter of policy; it is essential for safeguarding public health and wellbeing. Without decisive action, the repercussions of inaction could be devastating, not only for healthcare workers but for the millions who rely on these essential services.