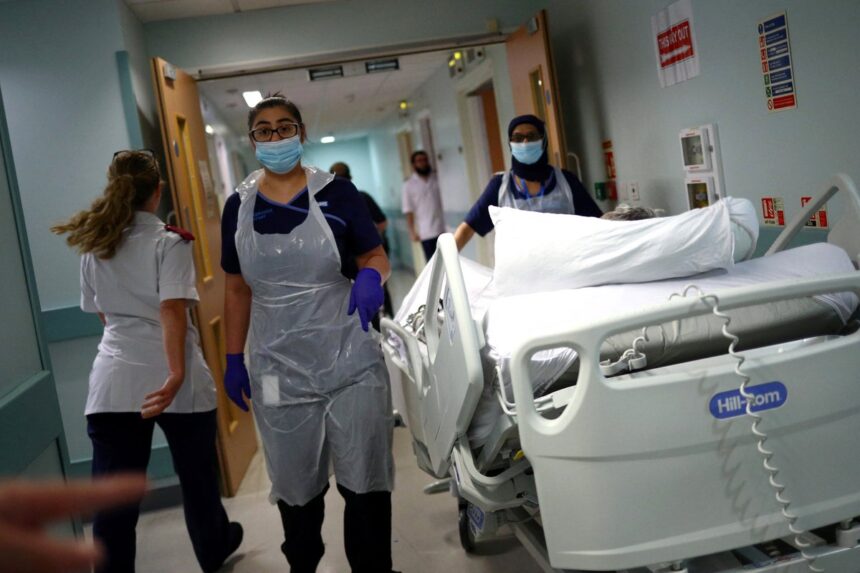
The National Health Service (NHS) is currently in a precarious position, with top health professionals expressing grave concerns over its ability to withstand another pandemic. As emergency departments grapple with overcrowding, record waiting lists, and a substantial strain on resources, the looming spectre of a new health crisis could expose the service’s vulnerabilities even further.
A Fraying Healthcare System
Leading figures in the medical community have issued stark warnings regarding the NHS’s current state. Overwhelmed emergency departments and an alarming increase in corridor care have left hospitals ill-prepared to manage not only everyday demands but also the potential influx of patients that could accompany a future pandemic. The situation is significantly worse now than it was prior to the Covid-19 crisis, with health leaders highlighting a concerning absence of effective planning for future health emergencies.
Dr Ian Higginson, president of the Royal College of Emergency Medicine, articulated the severity of the situation, stating, “Our hospitals are in a much more perilous state than they were before the last pandemic.” He emphasised that the current pressures on the system could easily lead to a breakdown, indicating that it takes minimal strain to push hospitals to their limits.
As the latest report from the Covid Inquiry is set to reveal the profound impact of the pandemic on the NHS, it is expected to detail harrowing accounts from frontline workers. The report is anticipated to depict conditions resembling “scenes from hell,” where resources were stretched to breaking point, and staff faced unimaginable challenges.
Alarming Statistics Highlight the Crisis
Recent NHS data underscores the gravity of the current situation. In January 2026, a staggering 71,517 patients endured waits exceeding 12 hours in Accident and Emergency departments—an increase from just 627 in January 2019. Furthermore, surgical waiting lists have surged to 7.2 million, up from 4.27 million pre-pandemic. Mental health services are equally strained, with nearly 1.8 million individuals awaiting care, and approximately 1.1 million people waiting for community health services.

Dr Vicki Price, president of the Society of Acute Medicine, reinforced the message that the NHS is not equipped for another pandemic. “If a condition similar to Covid-19 were to re-emerge, it would be disastrous for both patients and staff,” she warned, citing the ongoing challenges of managing an overstretched health system.
The Call for Preparedness
The Covid Inquiry, led by Baroness Heather Hallett, has revealed alarming insights regarding the NHS’s preparedness for future crises. During the inquiry, former NHS England medical director Sir Stephen Powis expressed his fears that the healthcare system could buckle under pressure once more, leading to rationed care and poor outcomes. Reports of inadequacies in protective equipment and the tragic loss of 860 healthcare workers during the pandemic serve as a stark reminder of the need for comprehensive planning.
Dr Shondipon Laha, president of the Intensive Care Society, lamented the rapid loss of lessons learned during the pandemic. He cautioned that the principles established for effective crisis response are not being systematically applied to current planning. “What we’re witnessing is a lack of application of the lessons we should have learned,” he stated, urging for a reinstatement of systems that effectively track available critical care beds.
The Human Cost of Burnout
As the NHS continues to navigate these challenges, healthcare workers are facing unprecedented levels of burnout. Dr Price highlighted the fatigue that pervades the workforce, noting that while staff previously went “above and beyond” during the pandemic, current conditions have led to increased exhaustion. The 2023 NHS staff survey revealed that over one-third of employees reported feeling burnt out, with only 32 per cent believing there are sufficient staff in their organisations.

Dr Laha acknowledged that intensive care unit personnel are sacrificing their well-being for their patients, a situation that has led to a significant toll on mental health. He warned, “We are at a worse point than we were during the original pandemic.”
In response to these concerns, a spokesperson for the Department of Health and Social Care (DHSC) asserted that the government is committed to revitalising the NHS through substantial investments and reforms. They highlighted recent progress in reducing waiting lists and improving treatment timelines, while also emphasising the importance of pandemic preparedness.
Why it Matters
The NHS stands as a crucial pillar of public health in the UK. Its current struggles reflect not only a looming crisis in healthcare delivery but also a broader challenge in safeguarding the health of the nation. As the threat of future pandemics remains, the need for strategic planning, adequate resource allocation, and a focus on staff well-being has never been more critical. The lessons learned from Covid-19 must be heeded to ensure that the NHS is not only able to survive but to thrive in the face of future health emergencies.