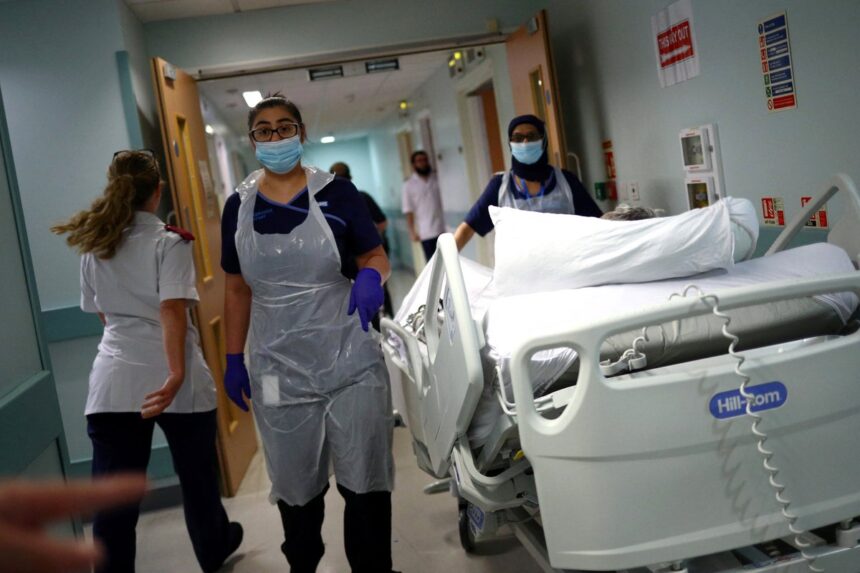
The National Health Service (NHS) is currently facing unprecedented pressures that have left it ill-equipped to handle another pandemic, according to senior medical professionals. With emergency departments overwhelmed, corridor care becoming the norm, and waiting lists soaring to alarming levels, the current state of the NHS is far more precarious than it was prior to the Covid-19 crisis. This stark warning comes just ahead of the latest findings from the Covid Inquiry, which is set to reveal the traumatic experiences endured by NHS staff and patients alike during the pandemic.
A System Under Siege
Health leaders are sounding the alarm over the dire situation within the NHS, characterising it as “perilous.” They report that hospitals are struggling to manage everyday patient demands, let alone the added stress of another health crisis. Dr Ian Higginson, president of the Royal College of Emergency Medicine, expressed his concern, stating, “Our hospitals are in a much more perilous state than they were before the last pandemic.” He noted that emergency departments are overcrowded and that a significant influx of patients could quickly overwhelm the system.
Recent NHS statistics underscore the severity of the situation: over 71,500 patients waited more than 12 hours in accident and emergency departments in January 2026, a staggering increase from just 627 in January 2019. Additionally, surgery waiting lists have ballooned to 7.2 million, a sharp rise from 4.27 million in 2019. Mental healthcare services are also struggling, with nearly 1.8 million people awaiting treatment.
The Lessons Unlearned
As the Covid Inquiry, led by Baroness Heather Hallett, prepares to release its findings, many health professionals are voicing their frustrations over a perceived failure to learn from past mistakes. Dr Shondipan Laha, president of the Intensive Care Society, highlighted that despite the hard-earned lessons from the pandemic, they have been rapidly forgotten. He warned, “It’s not just about being ready for a pandemic. It’s being ready for a war.” The lack of a robust preparedness plan is troubling, especially given the NHS’s current state.

Another area of concern is the absence of a national system to monitor available critical care beds, which was implemented during the pandemic but has since been discarded. Dr Laha emphasised the need for this system to be reinstated, asserting, “Anything that can be stopped has been stopped.” With the NHS currently navigating a tight economic landscape, some trusts are even considering reducing intensive care unit (ICU) bed numbers, a move that could have dire consequences.
The Human Cost of Overstretching
The impact of these systemic issues is being felt acutely by NHS staff, many of whom are experiencing burnout at unprecedented levels. Dr Vicki Price, president of the Society of Acute Medicine, pointed out that hospitals are currently operating with more patients than available beds, which exacerbates the strain on healthcare professionals. “If you have a condition that’s just like Covid-19, it will be a disaster for all the patients and staff working in those departments,” she warned.
Staff members are increasingly fatigued; a recent NHS survey revealed that over a third of employees reported feeling burnt out. This is compounded by financial cutbacks that have only intensified the pressures on the workforce. Dr Laha described how ICU staff are sacrificing their quality of life, working extra hours to meet the demands of patient care, leading to a significant decline in morale and well-being.
Preparing for the Unknown
As the NHS grapples with these immediate challenges, the question arises: what is being done to prepare for the next potential crisis? Baroness Hallett’s upcoming report will explore this very issue, assessing how the NHS has responded to Covid-19 and what lessons have been integrated into current practices.

For many health leaders, the fear is that unless significant changes are made, the NHS will find itself in an even more precarious position should another pandemic arise. Professor Mumtaz Patel, president of the Royal College of Physicians, lamented the “hideous” increase in corridor care, stating that the “completely broken” social care sector is exacerbating the crisis further.
Why it Matters
The current state of the NHS is not just a reflection of systemic inefficiencies; it represents a pressing public health concern that affects the entire population. With hospitals already stretched thin, the implications of being unprepared for future health emergencies could be catastrophic. As leaders in healthcare call for immediate action and comprehensive planning, it is imperative that the government and health authorities heed these warnings. The health and safety of the population depend on a resilient NHS that is equipped to face whatever future challenges may arise.